6 results
Antibiotic-prescribing practices and associated outcomes after common urologic procedures in an integrated healthcare system
- Daniel Livorsi, Bibiana Ruiz Granado, Bruce Alexander, Ryan Steinberg, Vignesh Packiam, Brian Lund
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
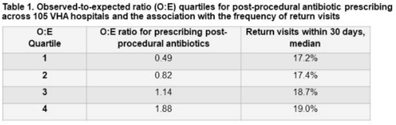
Background: Many urologists continue antibiotics after common urologic procedure beyond the timeframes recommended by professional guidelines. In this study, we sought to evaluate the association between postprocedural antibiotic use and patient outcomes. Methods: We identified all patients who underwent 1 of 3 urologic procedures (transurethral resection of bladder tumor [TURBT], transurethral resection of prostate [TURP], and ureteroscopy) within the Veterans’ Health Administration (VHA) between January 1, 2017, and June 30, 2021. A postprocedural antibiotic was any antibiotic potentially used for a urinary tract–related indication that was prescribed for administration after the day of the procedure. Outcomes were captured within 30 days of the procedure and included (1) return visits, defined as any emergency department or urgent care encounter or hospital readmission, and (2) Clostridium difficile infection (CDI), defined as a positive test for C. difficile and the prescription of an anti-CDI antibiotic. We used log-binomial models with risk adjustment to determine the association between postprocedural antibiotic use and outcomes. We constructed hospital-level observed-to-expected ratios for postprocedural antibiotic use, and we used these models to calculate the probability of each patient receiving postprocedural antibiotics. Results: Overall, we identified 74,629 patients; 98% were male; the mean age was 70 years (SD, 10). Among them, 50% underwent TURBT, 28% underwent TURP, and 23% underwent ureteroscopy. A postprocedural antibiotic was prescribed to 25,738 (35%) cases for a median duration of 3 days (IQR, 3–6). Return visits occurred in 13,489 patients (18%), and CDI occurred in 104 patients (0.1%). Patients exposed to postprocedural antibiotics had 16% more return visits (RR, 1.16; 95% CI, 1.13–1.20) and more than twice as much CDI (RR, 2.22; 95% CI, 1.51–3.26) than patients not exposed to postprocedural antibiotics. In log-binomial risk-adjusted analysis, the risk of return visits did not differ between the 2 groups (RR, 1.00; 95% CI, 0.97–1.04) but the risk of CDI was higher in patients who received post-procedural antibiotics (RR, 1.87; 95% CI, 1.00–3.51). Hospitals (n = 105) varied widely in their observed-to-expected ratios for prescribing postprocedural antibiotics, and the frequency of return visits was similar regardless of the frequency at which postprocedural antibiotics were prescribed (Table 1). Conclusions: Postprocedural antibiotics were prescribed beyond recommended intervals after more than one-third of common urologic procedures, with a large degree of variability across hospitals. The use of postprocedural antibiotics was not associated with fewer return visits but was associated with a nonsignificant increase in CDI risk. Efforts to reduce postprocedural antibiotics are needed.
Funding: Yes
Disclosures: This work was funded, in part, by the Merck Investigator Studies Program. This work was also supported by a Career Development Award (DJL) from the VA Health Services Research and Development Service (CDA 16-204) and by the Iowa City VA Health Care System, Department of Pharmacy Services.
24 - Precision Behavioral Management (PBM): A Novel Genetically Guided Therapy to Combat Reward Deficiency Syndrome (RDS) Relevant to the Opiate Crisis
- from Part V - Ongoing and Future Research Directions
-
- By Kenneth Blum, Alphonse Kenison Roy, Arwen Podesta, Edward J. Modestino, Bruce Steinberg, Marjorie C. Gondré-Lewis, David Baron, Panayotis K. Thanos, Lisa Lott, Sampada Badgaiyan, Jessica Valdez Ponce, Brent Boyett, David Siwicki, Mark Moran, Drew Edwards, Thomas McLaughlin, Eric R. Braverman, Thomas A. Simpatico, Mary Hauser, Bernard William Downs, Rajendra D. Badgaiyan
- Edited by Steve Sussman, University of Southern California
-
- Book:
- The Cambridge Handbook of Substance and Behavioral Addictions
- Published online:
- 13 July 2020
- Print publication:
- 06 August 2020, pp 297-306
-
- Chapter
- Export citation
-
Summary
Reward Deficiency Syndrome (RDS) is an umbrella term for all drug and nondrug addictive behaviors, due to a dopamine deficiency, “hypodopaminergia.” There is an opioid-overdose epidemic in the USA, which may result in or worsen RDS. A paradigm shift is needed to combat a system that is not working. This shift involves the recognition of dopamine homeostasis as the ultimate treatment of RDS via precision, genetically guided KB220 variants, called Precision Behavioral Management (PBM). Recognition of RDS as an endophenotype and an umbrella term in the future DSM 6, following the Research Domain Criteria (RDoC), would assist in shifting this paradigm.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
A Multicenter Study on Optimizing Piperacillin-Tazobactam Use: Lessons on Why Interventions Fail
- Robert P. Gaynes, Carolyn V. Gould, Jonathan Edwards, Theresa L. Antoine, Henry M. Blumberg, Kathryn DeSilva, Mark King, Alice Kraman, Jan Pack, Bruce Ribner, Ulrich Seybold, James Steinberg, John A. Jernigan
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 30 / Issue 8 / August 2009
- Published online by Cambridge University Press:
- 02 January 2015, pp. 794-796
- Print publication:
- August 2009
-
- Article
- Export citation
-
We examined interventions to optimize piperacillin-tazobactam use at 4 hospitals. Interventions for rotating house staff did not affect use. We could target empiric therapy in only 35% of cases. Because prescribing practices seemed to be institution specific, interventions should address attitudes of local prescribers. Interventions should target empiric therapy and ordering of appropriate cultures.
Use of a Mandatory Declination Form in a Program for Influenza Vaccination of Healthcare Workers
- Bruce S. Ribner, Cynthia Hall, James P. Steinberg, William A. Bornstein, Rosette Chakkalakal, Amir Emamifar, Irving Eichel, Peter C. Lee, Penny Z. Castellano, Gilbert D. Grossman
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 29 / Issue 4 / April 2008
- Published online by Cambridge University Press:
- 02 January 2015, pp. 302-308
- Print publication:
- April 2008
-
- Article
- Export citation
-
Objective.
To evaluate the utility and impact of using a declination form in the context of an influenza immunization program for healthcare workers.
Methods.A combined form for documentation of vaccination consent, medical contraindication(s) for vaccination, or vaccination declination was used during the 2006-2007 influenza season in a healthcare system employing approximately 9,200 nonphysician employees in 3 hospitals; a skilled nursing care facility; a large, multisite, faculty-practice plan; and an administrative building. Responses were entered into a database that contained files from human resources departments, which allowed correlation with job category and work location.
Results.The overall levels of influenza vaccination coverage of employees increased from 43% (3,892 of 9,050) during the 2005-2006 season to 66.5% (6,123 of 9,214) during the 2006-2007 season. Of 9,214 employees, 1,898 (20.6%) signed the declination statement. Among the occupation groups, nurses had the lowest rate of declining vaccination (13.2% [393 of 2,970]; P < .0001), followed by pharmacy personnel (18.1% [40 of 221]), ancillary personnel with frequent patient contact (21.9% [169 of 771), and all others (24.7% [1,296 of 5,252]). Among the employees who declined vaccination, nurses were the least likely to select the reasons “afraid of needles” (3.8% [15 of 393], vs. 9.1% [137 of 1,505] for all other groups; P < .001) and “fear of getting influenza from the vaccine” (13.5% [53 of 393], vs. 20.5% [309 of 1,505]; P = .002). Seven pregnant nurses had been advised by their obstetricians to avoid vaccination. When declination of influenza vaccination was analyzed by age, 16% of personnel (797 of 4,980) 50 years of age and older declined to be vaccinated, compared with 26% of personnel (1,101 of 4,234) younger than 50 years of age {P < .0001).
Conclusions.Implementing use of the declination form during the 2006-2007 influenza season was one of several measures that led to a 55% increase in the acceptance of influenza vaccination by healthcare workers in our healthcare system. Although we cannot determine to what degree use of the declination form contributed to the increased rate of vaccination, use of this form helped the vaccination program assess the reasons for declination and will help to focus future vaccination campaigns.
Knowledge, Attitudes, and Behaviors Regarding Piperacillin-Tazobactam Prescribing Practices: Results From a Multicenter Study
- Theresa L. Antoine, Amy B. Curtis, Henry M. Blumberg, Kathryn DeSilva, Mesfin Fransua, Carolyn V. Gould, Mark King, Alice A. Kraman, Jan Pack, Bruce Ribner, Ulrich Seybold, James P. Steinberg, Jane B. Wells, Ronda L. Sinkowitz-Cochran, Denise Cardo, John A. Jernigan, Robert P. Gaynes
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 27 / Issue 11 / November 2006
- Published online by Cambridge University Press:
- 21 June 2016, pp. 1274-1277
- Print publication:
- November 2006
-
- Article
- Export citation
-
We investigated knowledge, attitudes, and behaviors of prescribers concerning piperacillin-tazobactam use at 4 Emory University-affiliated hospitals. Discussions during focus groups indicated that the participants' perceived knowledge of clinical criteria for appropriate piperacillin-tazobactam use was inadequate. Retrospective review of medical records identified inappropriate practices. These findings have influenced ongoing interventions aimed at optimizing piperacillin-tazobactam use.




